Abdominal Aortic Aneurysm – The triple A to avoid
Tuesday, December 8, 2020
As a common acronym for the American Automobile Association, Triple A or AAA can be a lifesaver in times of automotive problems that often find motorists on the side of the road. In contrast, an Abdominal Aortic Aneurysm – also known as Triple A or AAA – is one of the most common vascular issues that can prove life threatening in some cases.
Abdominal aortic aneurysms (AAAs) are typically caused by progressive weakening of the aortic wall that creates a “ballooning” of the blood vessel. While most aneurysms are asymptomatic, they may expand in size and eventually rupture if not diagnosed and treated.
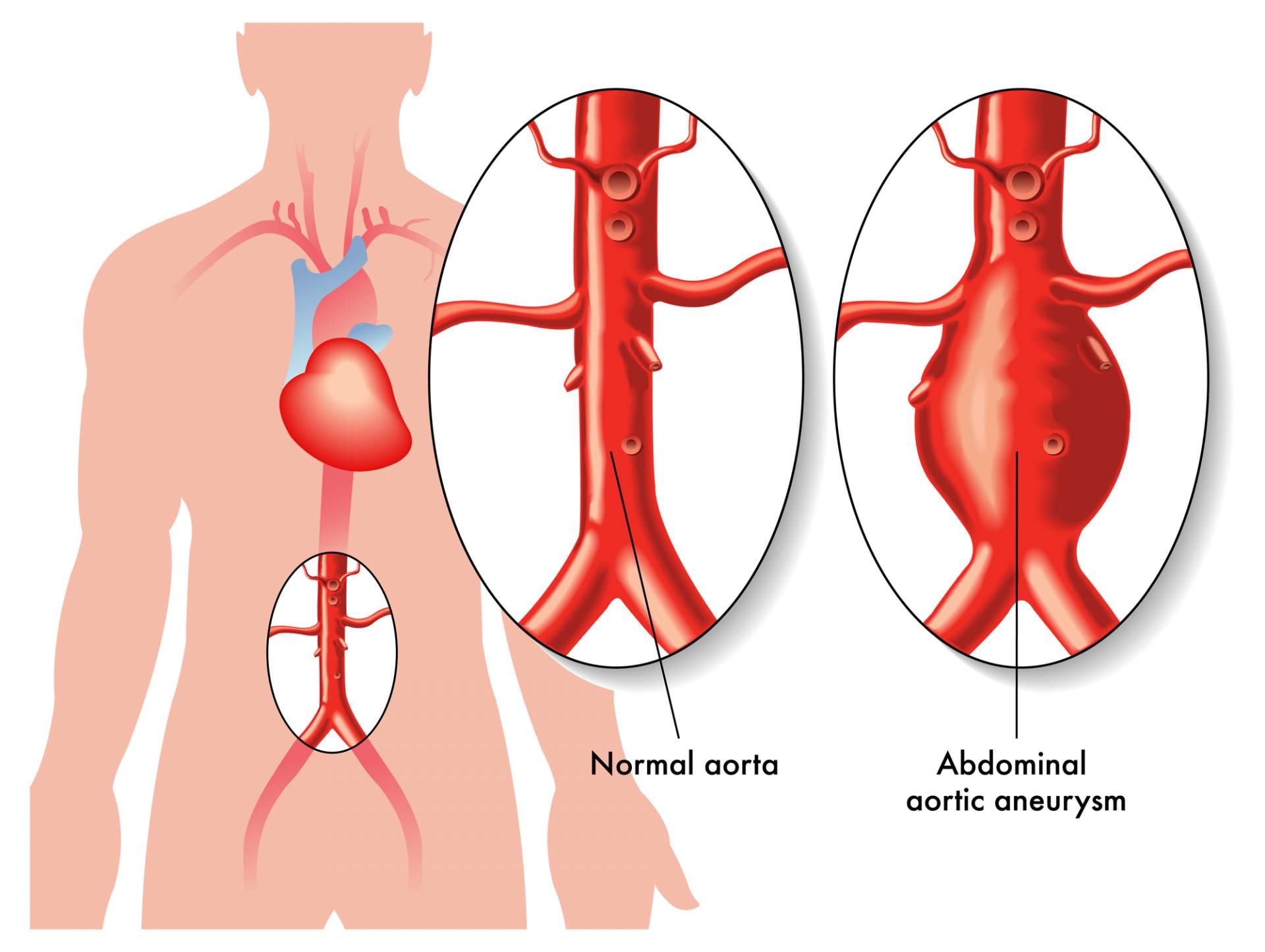
Aneurysms occur most often in the aorta, the main artery of the chest and abdomen, which carries blood from the heart to all parts of the body.
Like many silent-but-deadly health issues, there are no major symptoms for AAA in most cases as it often grows slowly. Occasionally, patients may feel abdominal, back or side pain, which can be signs of impending rupture. Some patients may also experience nausea or a pulsating abdominal mass, which are also common symptoms.
When it comes to diagnosing abdominal aortic aneurysms, statistics show that 75 percent of aneurysms that are discovered are detected from diagnostic tests (such as x-rays) that were scheduled for other health problems. While AAAs can be detected by physical exam, most are diagnosed by ultrasound or computed tomography (CT) scan. Both are non-invasive, outpatient procedures designed to measure the size of AAAs, and determine the best treatment for the patient. What is key to remember is that when an aortic aneurysm is diagnosed early, treatment is typically safe and effective, and rupture of the aneurysm is preventable.
According to statistics from the Mayo Clinic, abdominal aortic aneurysms are responsible for three million cases per year, and are most common in older men and smokers. In addition to knowing the few symptoms of an abdominal aortic aneurysm, there are many risk factors that can cause or advance the development of AAAs. The most important risk factors are:
- An age over 60 years
- Tobacco use
- Family history of AAA
- History of heart disease or peripheral artery disease (PAD)
- High blood pressure (hypertension)
Some quick facts to keep in mind about abdominal aortic aneurysms are:
- The risk of AAA increases with age
- Tobacco users are eight times more likely to be affected than non-users
- AAAs are between five to 10 times more common in men than in women
- There are approximately 15,000 deaths per year related to the rupture of an aneurysm
- Ruptured aneurysms are the 10th leading cause of death in men over 50 in the country
Most AAAs typically develop as the result of a weakening of elastin and collagen in the aortic wall. In addition, inflammation associated with atherosclerosis can accelerate the degenerative process. Some of the body’s naturally occurring enzymes may cause the breakdown of collagen and elastin in the aortic wall. An excess of these enzymes or conditions that activate the enzymes may cause the formation or growth of an aneurysm.
When it comes to the treatment of abdominal aortic aneurysms, size truly does matter. Small aneurysms – less than 4.5-5cm – can generally be safely observed. As the aneurysm size begins to increase beyond this level, to greater than 5.5cm for instance, the risk of rupture increases exponentially and surgery is advised. Other factors that determine whether surgery is necessary is the rate of growth of the aneurysm and whether the patient has any symptoms such as abdominal or back pain.
In the past, the main treatment for large AAAs was open surgery through an incision in the abdominal wall and replacement of the aneurysm with a synthetic graft. Today, most aneurysms can be treated in a minimally invasive manner with stent grafts placed through two small incisions in the groin. This is usually a well-tolerated procedure with most patients requiring only one or two days in the hospital following surgery, and a quicker return to work.
Ultimately, the combination of early diagnosis, regular monitoring and appropriately timed treatment can prevent deaths from ruptured abdominal aortic aneurysms.









Thanks to his knowledge and guidance, I experienced significant improvement and, ultimately, complete healing. His approach was thorough, professional, and reassuring, which made the entire process much easier to handle. I truly appreciated how he took the time to explain every step and answer all my questions patiently. Dr. Ikpoko on Youtube didn’t just treat a medical condition; he restored my confidence and quality of life. I feel healthier, happier, and more empowered today because of his dedication. I wholeheartedly recommend Dr. Ikpoko to anyone seeking expert help for oral herpes or similar conditions. Website: https://drikpoko.wixsite.com/herbs Or email: Drikpoko@gmail.com Thank you so much, Dr. Ikpoko, for your outstanding care and for giving me a fresh start! Thursday, November 27, 2025
Last year, hoping for additional support, I decided to try a herbal treatment program from NaturePath Herbal Clinic. Honestly, I was skeptical at first, but within a few months, I began to feel some changes. My fatigue lessened, my digestion felt better, and overall I felt more balanced and healthier. I also regained much of my energy and confidence. It’s been a meaningful experience, and I feel more like myself again.If you or a loved one is dealing with Hepatitis B, you might consider exploring complementary approaches that feel right for you. This was simply my personal experience. You can visit their website or contact them at www.naturepathherbalclinic.com ,
info@naturepathherbalclinic.com Monday, December 8, 2025
Despite my visit to several doctors my health wasn't getting better, all they could say is for me to stay on the treatment. At the verge of giving up, I went to the internet to search for a treatment on my own at least. But I found a cure instead. On the internet, I read a testimony of a lady who had herpes. She shared an e-mail address of the Doctor. Luckily everything seemed to be okay after I took Herbal Medicine. I wish I could say that’s the end of it because I haven't had any symptoms since then. Do not expose yourself to more danger, use a herbal remedy that is safe and effective. If interested, contact Dr Ikpoko via email: drikpoko@gmail.com Whatsapp +2348108298045 https://drikpoko.wixsite.com/herbs You are the best Doctor sir. Wednesday, December 10, 2025
Sunday, December 14, 2025
Don’t be too skeptical to take good care of yourself because you heard our Government said there is no cure to Herpes Virus, That was my first thought until I finally met a great herbalist from west Africa Nigeria and his name is Dr Ikpoko on YouTube, THE CAREGIVER, His Herbs 🌿 work very effectively but it has no side effects. All I want you to do is to reach out to him via whatsapp: +2348108298045, drikpoko@gmail.com or visit his website https://drikpoko.wixsite.com/herbs and stop believing in our bad Government because they didn’t want to help us then we need to help ourselves and earlier we realize this and earlier it will be better for us all, HSV have a complete cure because I was cure from this so called Hsv-1 After completing the herbal medication that was ship to me by herbal Doc. Ikpoko on YouTube channel, for three weeks and it has been two months. I have not gotten any symptoms or outbreaks in my body, GLORY to God that he has sent a wonderful and kind hearted man to me in regaining my health back to me. Tuesday, January 6, 2026
Wow what a good God I am so excited to tell you all how I become a millionaire I’m a woman of faith I was reading a comment on google where I meet a man sharing how Dr UYI cast a spell for him and he get his wife back after the spell I was interested I have to do research when I was doing the research I got so many testimony about this same man call Dr UYI how he help people to win lottery how he help people to get there ex back how he help people to do so many things I was happy and I contact him to help me win the lottery when I contact him and he told me what to do and after I did what he ask me to do he den gave me a lottery number to play and told me to go and buy ticket after playing the game I was so surprise the game come out good and I won the sum of 90, 000,000 dollars i was amazed and promise to share it to the people around me if anyone is willing to play the mage lottery it should contact Dr UYI so he can give you the right number to play thanks to you Dr UYI I’m so so grateful contact Dr UYI via drzukalottospelltemple@gmail.com OR WhatsApp on +17174154115 Friday, January 9, 2026
https://drosaluherbalhome.wixsite.com/drosaluherbshome Saturday, January 17, 2026
Wednesday, January 21, 2026
Wednesday, January 21, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Thursday, January 22, 2026
https://drosaluherbalhome.wixsite.com/drosaluherbshome Tuesday, January 27, 2026
telegram ----- https://t.me/solution59
Friday, January 30, 2026
I’m so happy right now, It is amazing how quickly Dr. Excellent brought my husband back to me. My name is Heather Delaney. I married the love of my life Riley on 10/02/15 and we now have two beautiful girls Abby & Erin, who are conjoined twins, that were born 07/24/16. My husband left me and moved to be with another woman. I felt my life was over and my kids thought they would never see their father again. I tried to be strong just for the kids but I could not control the pains that tormented my heart, my heart was filled with sorrows and pains because I was really in love with my husband. I have tried many options but he did not come back, until i met a friend that directed me to Dr. Excellent a spell caster, who helped me to bring back my husband after 11hours. Me and my husband are living happily together again, This man is powerful, contact Dr. Excellent if you are passing through any difficulty in life or having troubles in your marriage or relationship, he is capable of making things right for you. Don't miss out on the opportunity to work with the best spell caster. Here his contact. Call/WhatsApp him at: +2348084273514 "Or email him at: Excellentspellcaster@gmail.com ,For more information visit his website:https://drexcellentspellcaster.godaddysites.com
Thursday, February 5, 2026
Welcome to Good Life Bitcoin Trading
I am a bitcoin professional trader, and I always win my trade with my best
trading platform, so are you looking for a professional trader or looking for
someone that can help you invest and trade your Bitcoin for more profit to be
made? With and 8 hours of investment profit plans.
Do you know you can grow your money by investing in Bitcoin and get profit by
helping you to trade, Email us for more info melodygoodlife617@gmail.com
My investment plans;
Invest 0 X 8=Core: Blog,000
Invest 0 X 8=,000
Invest ,000 X 8=,000
Invest ,500 X 8=,000
Invest $,2,000 X 8=,000
Invest ,000 X 8=,000
Contact us today let's teach you how you can get that done with proof on my
trading platform by investing and make your profit in 8-Hours..
E-mail Address: melodygoodlife617@gmail.com
Melody Good Life.
A Try We Convince You With Good Life Investment.
Thursday, February 5, 2026
WhatsApp. +2349073130326
Email: dragbonhaleherbalhome@gmail.com
God bless you. Thursday, February 5, 2026
WhatsApp. +2349073130326
Email: dragbonhaleherbalhome@gmail.com
God bless you🙏 Thursday, February 5, 2026
FB Page: https://www.facebook.com/share/1D5myk4Bxb/
Youtube Page: https://www.youtube.com/@JatoLoveSpell
..... Friday, February 6, 2026
FB Page: https://www.facebook.com/share/1D5myk4Bxb/
Youtube Page: https://www.youtube.com/@JatoLoveSpell
. Friday, February 6, 2026
HIV/AIDS,
SHINGLES,
CANCER,
HUMAN PAPILLOMA VIRUS,
ASTHMA,
DIABETES
BARRENNESS/INFERTILITY P*NIS ENLARGEMENTSPELL COUNSELING.
You Can decide to reach Herbalist Razor on his Email address : drrazorherbalhome@gmail.com . Cell Phone/Whatsapp Number +2349065420442 . Saturday, February 7, 2026
his Email: drahonsie00@gmail.com
WhatsApp: +2348039482367
https://drahonsie002.wixsite.com/dr-ahonsie Sunday, February 8, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Monday, February 9, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Tuesday, February 10, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa Wednesday, February 11, 2026
Read more on his website:
https://ancientspellcast.wordpress.com
WhatsApp: +2347070518515 Wednesday, February 11, 2026
Everything that Dr Timothy said about the medication are true. I am full with Joy to see my loving sister strong and healthy again. Contact him on: goodhealthherbalfoundation@yahoo.com OR WhatsApp +2349019250610
website https://5dc41d5b6d60d.site123.me Wednesday, February 11, 2026
Diabetes, Lupus, HPV, Gout, Hepatitis A,B, PCOS, Infertility, HIV/AIDS, CANCER, WART Wednesday, February 11, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa
Wednesday, February 11, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa
Wednesday, February 11, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa Thursday, February 12, 2026
Thursday, February 12, 2026
The rise of digital currencies has reshaped global finance, offering new opportunities alongside new risks. Lost access, unauthorized transfers, and deceptive platforms continue to affect thousands of individuals and organizations, leaving many uncertain about where to turn.
TREK Tech Corp has become the trusted leader in digital asset recovery, known for its lawful, transparent, and results driven approach. With thousands of successful cases worldwide, TREK Tech Corp provides clients with more than recovery it offers justice, integrity, and peace of mind. Lawful Precision, Real Results
Unlike unverified operators that exploit victims with false promises, TREK Tech Corp is defined by legitimacy. The firm’s “no upfront fee” policy ensures clients only pay after a successful outcome, protecting them from secondary losses. Each case is evaluated carefully, with realistic expectations and tailored strategies.
TREK Tech Corp combines advanced blockchain forensics with proprietary tools like Cross-Chain Mapping Blockchain (CCMB) to trace assets across multiple blockchains, mixers, and offshore exchanges. This technology, paired with human expertise, makes it possible to solve complex cases often considered irretrievable. Backed by Law and Global Collaboration
What sets TREK Tech Corp apart is its active partnership with global authorities. By working with organizations such as the FBI, Interpol, and national cybersecurity agencies, TREK Tech Corp ensures that recoveries are lawful, enforceable, and credible. Comprehensive Services
TREK Tech Corp provides solutions for a wide range of challenges, including:
Digital asset recovery across major blockchains
Wallet access restoration (Ledger, Trezor, MetaMask, Trust Wallet)
Investment and platform-related losses
NFT restoration and exchange account support
Contact TREK Tech Corp
If you’ve experienced digital asset loss, time is critical. TREK Tech Corp is ready to help you act quickly and effectively.
Email: trektechcorp1@gmail.com
Email: trektechcorp@consultant.com
Website: (https://trektechcorp.net)
With TREK Tech Corp, recovery is built on lawful precision, proven results, and unwavering integrity.
Thursday, February 12, 2026
At 49, single after a long marriage ended, I thought I’d finally met “the one.” ‘Marcus’—charming consultant working abroad—filled my days with loving texts, voice notes that made me blush, and promises of a shared life once his project wrapped. He showed me his crypto trades exploding, said we could multiply our savings together on his “exclusive vetted platform” for couples planning forever—28% monthly returns, easy and safe. My heart believed every word. I sent my 8K nest egg in crypto. Then silence. Blocked everywhere. I curled up in the dark, clutching my phone, sobbing until my chest hurt—used, humiliated, completely broken. At 3 a.m., barely able to type, I reached JetWebHackers. They jumped on it, followed the crypto trail with fierce determination, recovered every cent in weeks. Funds returned… I sat there stunned, tears of relief pouring down. For the first time in months, I could breathe without pain. They didn’t just get my money back—they reminded me that kindness still exists. If a crypto romance scam left you shattered, please reach out. JetWebHackers are the real ones who lift women like me back up.#JetWebHackers
EMAIL: support@jetwebhackers.com
WhatsApp: +1 (260) 228-9998
Thursday, February 12, 2026
At 49, single after a long marriage ended, I thought I’d finally met “the one.” ‘Marcus’—charming consultant working abroad—filled my days with loving texts, voice notes that made me blush, and promises of a shared life once his project wrapped. He showed me his crypto trades exploding, said we could multiply our savings together on his “exclusive vetted platform” for couples planning forever—28% monthly returns, easy and safe. My heart believed every word. I sent my 8K nest egg in crypto. Then silence. Blocked everywhere. I curled up in the dark, clutching my phone, sobbing until my chest hurt—used, humiliated, completely broken. At 3 a.m., barely able to type, I reached JetWebHackers. They jumped on it, followed the crypto trail with fierce determination, recovered every cent in weeks. Funds returned… I sat there stunned, tears of relief pouring down. For the first time in months, I could breathe without pain. They didn’t just get my money back—they reminded me that kindness still exists. If a crypto romance scam left you shattered, please reach out. JetWebHackers are the real ones who lift women like me back up.#JetWebHackers
EMAIL: support@jetwebhackers.com
WhatsApp: +1 (260) 228-9998
Thursday, February 12, 2026
+2349064159687 or Email odiagbebello@gmail.com
Friday, February 13, 2026
If you have been taking conventional medicines for that Herpes infection and you are still having those re-occurring outbreaks, why don’t you try Herbal Medicines and see it get cured in weeks. For more information, send me ON WhatsApp
+2349064159687 or Email odiagbebello@gmail.com Friday, February 13, 2026
+2349064159687 or Email odiagbebello@gmail.com
Saturday, February 14, 2026
+2349064159687 or Email odiagbebello@gmail.com
Saturday, February 14, 2026
+2349064159687 or Email odiagbebello@gmail.com
Thanks for reading. and God bless you🙏 Saturday, February 14, 2026
https://dromolaherbalhome.wixsite.com/website
Email: dr.omolaherbalhome@gmail.com
Saturday, February 14, 2026
Sunday, February 15, 2026
WhatsApp. +2349073130326
Email: dragbonhaleherbalhome@gmail.com
God bless you🙏 Sunday, February 15, 2026
Monday, February 16, 2026
Monday, February 16, 2026
Monday, February 16, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Tuesday, February 17, 2026
Tuesday, February 17, 2026
I thought my life had nothing to offer anymore because life became meaningless to me because I had HERPES VIRUS, the symptoms became very severe and bold and made my family run from and abandon me so they won't get infected. I gave up everything, my hope, dreams,vision and job because the doctor told me there's no cure. I consumed so many drugs but they never cured me but hid the symptoms inside me making it worse. I was doing some research online someday when I came across testimonies of some people of how Dr.Akhimien cured them from HERPES VIRUS, I never believed at first and thought it was a joke but later decided to contact him on the details provided and when I messaged him we talked and he sent me his herbal medicine and told me to go for a test after two weeks. Within 9 days of medication the symptoms disappeared and when I went for a test Lo and behold I was NEGATIVE by the Doctor Who tested me earlier. Thank you Dr.Akhimien because I forever owe you my life and I'll keep on telling the world about you. If you are going through the same situation, worry no more and contact DR Akhimien via website: https://drakhiniemodion.wixsite.com/drakhimien
or email: drakhiniemodion@gmail.com ,his
WhatsApp him via +2349133157031 Wednesday, February 18, 2026
(+2348056484618) email himon: Luckyseph1113@gmail.com, For immediately response… My Regard to Mr Joseph Lucky .............. Wednesday, February 18, 2026
If you have been taking conventional medicines for that Herpes infection and you are still having those re-occuring outbreaks, why don't you try Herbal Medicines and see it get cured in weeks. For more information, send me an
Email: ridvid8@gmail.com
Telegram: @wafri01
https://wa.me/447593340459
website: //ridvid8.wixsite.com/dr-ayo-herbs-home/about-5
Wednesday, February 25, 2026
Don’t be too skeptical to take good care of yourself because you heard our Government said there is no cure to Herpes Virus, That was my first thought until I finally met a great herbalist from west Africa Nigeria and his name is Dr Ikpoko on YouTube, THE CAREGIVER, His Herbs 🌿 work very effectively but it has no side effects. All I want you to do is to reach out to him via whatsapp: +2348108298045, drikpoko@gmail.com or visit his website https://drikpoko.wixsite.com/herbs and stop believing in our bad Government because they didn’t want to help us then we need to help ourselves and earlier we realize this and earlier it will be better for us all, HSV have a complete cure because I was cure from this so called Hsv-1 After completing the herbal medication that was ship to me by herbal Doc. Ikpoko on YouTube channel, for three weeks and it has been two months. I have not gotten any symptoms or outbreaks in my body, GLORY to God that he has sent a wonderful and kind hearted man to me in regaining my health back to me. Thursday, February 26, 2026
We are reliable and trusted vendors of Nembutal (Pentobarbital Sodium).We have established an excellent reputation over the years by providing our customers with excellent quality/ purity Nembutal. We offer pleasant and professional shipping experience with 100% discreet packaging and delivery worldwide. Our warehouse is unlimited. We sell Nembutal in Liquid form(50ml, 100ml, 250ml bottles)and in powder form ranging from 25g,50g,100g, etc. If you are looking to buy Nembutal Online, do not look any further. We have provided the safest and most accurate methods to buy Nembutal online and our service can be offered worldwide. Distance is not a barrier when ordering from us. We continuously invest in our service and upgrade on a daily basis to meet up with the demands of our customers. For your orders and more information you can reach us in the various ways listed below.
We offer a wide variety of pharmaceutical products that contain almost everything you need. Fast and discreet shipping quality 100% guaranteed, Express by UPS, FedEx, EMS with tracking number, no receipt required.
Ant-anxiety
Chronic Pain
Seizures
Depression
Migraines
Arthritis
Killing Cancer
Epilepsy
Post Traumatic stress
Disorder(pstd)
Diabetes
Crohn's Disease
Gout
Pain relief
Glaucoma
Opiod Dependence
Treating Alcohol Abuse
WhatsApp:+447401473736
Telegram: @Ranko3222
https://toprapidsolution.blogspot.com/
Note: we ship Nembutal 100% discreetly and expedited all over the world and we have a returns policy that offers our customers maximum satisfaction. We are available 24 hours a day to answer all your questions and also show you samples as long as you prove to be serious customer.
We are determined to give truly painful people real hope and lasting rest. We sell Nembutal powder and Nembutal Solution(Injectable). Simply indicate your age and weight, we will be able to provide you with exact information on price, delivery and payment.
When you order Nembutal online from us, we keep a close eye on details. We want to be sure of the dosage that will certainly be effective. You can purchase Nembutal online without any prescription and collect the shipped package without having to sign any papers. Shipping and delivery usually take a maximum of 3 days. All you have to do is provide some health related facts (for dosage estimates)
SERIOUS INQUIRIES ONLY
Tuesday, March 3, 2026
STOP STRUGGLING IN BED, TAKE BACK YOUR POWER TODAY!
DOCTOR AZIBA HERBAL MEDICINE is a fast acting, powerful natural male enhancement formula created for men who are fed up with embarrassment, weak erections, and disappointing bedroom performance. This proven herbal solution attacks sexual weakness, erectile dysfunction, low libido, and poor stamina at the root restoring your strength, confidence, and total dominance in bed.
This potent formula naturally boosts testosterone, ignites explosive sexual desire, and delivers rock hard erections that last longer than ever before. Experience renewed energy, unstoppable endurance, and complete control every time you step into the bedroom. Aging, stress, and fatigue will no longer control your sex life, YOU WILL.
Don’t let another night of failure damage your confidence or destroy your relationship.
Act now and experience the power trusted by real men to perform harder, stronger, and longer.
Results speak for themselves, satisfaction guaranteed.
Get in contact with Doctor Aziba for help via...
📧 Email: Priestazibasolutioncenter@gmail.com
📱 WhatsApp NOW: +2348100368288
Wednesday, March 4, 2026
Wednesday, March 4, 2026
You can also visit his websites Wednesday, March 4, 2026
Read on his website
drpeterspellcaster.mystrikingly.com/
WhatsApp +2348162247974 Thursday, March 5, 2026
Read on his website
WhatsApp +2348162247974 Thursday, March 5, 2026
WhatsApp:+2348142217151 Thursday, March 5, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Thursday, March 5, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256
2026 LOVE SPELL CASTER TO RESTORE YOUR BROKEN RELATIONSHIP WITHIN 24 HOURS
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Thursday, March 5, 2026
My Name is Nate from Ireland, I want to say thank you to Doctor Masako for the good thing he has done for me, Though am not sure if this is the best forum to show my joy and happiness for what he has done for me but i can’t hide happiness and my Joy so i have to share it with people, my marriage got crashed about two years ago and i tried all i could within my power but to no avail. I saw a post and testimonial about the good things Doctor Masako has been doing so I decided to give it a try. though he is always a busy man but when he responded back to my email, he gave me 24hours for my marriage to be restored really just like he said my marriage was restored since then I am happy and i am living happily i am so grateful, Doctor Masako you can always email him here: doctormasako@gmail.com or WHATSAPP +2349047144277 Website: doctormasako2.wixsite.com/drmasakospelltemple Thursday, March 5, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Friday, March 6, 2026
Whatsapp: +2349047144277 Saturday, March 7, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa
Saturday, March 7, 2026
website to make order now : https://drsikiesherbalcuremedicine.weebly.com/ Sunday, March 8, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa Sunday, March 8, 2026
Monday, March 9, 2026
My name is Andrea Meyer from the United State of America, and I am here to Share my testimony and experience with the herbal practitioner called Dr.Femi I meant online a few months ago who gave me some herbs that healed me completely from Herps and HSV-2. after suffering from this deadly disease for so many years.
And the good news is that he also have solutions to so many more diseases such as diabetes type2, cancer, HIV, Obesity, Arthritis infections of any kind and pregnancy related issues etc, and lots more I cannot mention.
I said to myself I cannot keep such good news to myself alone because I know so many of us are going through deadly illness out there and I decided to Share the good news to let you all know that there is still hope for you to get batter and that is why you must have to contact him through his email as soon as possible.
If interested kindly contact him for more information via email: drfemiherbalmedicines@gmail.com
Whatsapp on +2349153165215 Tuesday, March 10, 2026
Wednesday, March 11, 2026
If you’re looking to permanently eliminate HERPES, I highly recommend reaching out to Dr. Dan. You can contact him via WhatsApp at +447347220754 or email him at drdanhealingherbs@yahoo.com.
Don’t underestimate the powerful healing potential of herbs! Wednesday, March 11, 2026
You can contact him on his email: drriaria@gmail.com or call/WhatsApp him on +1 364 547-0111
Check out his website for more info:
https://drriaria.wixsite.com/website Thursday, March 12, 2026
website to make order now : https://drsikiesherbalcuremedicine.weebly.com/ Friday, March 13, 2026
1. Getting your lover or husband back
2. HIV/aids cure spell
3. Pregnancy spell
4. Money spell
5. Long life spell
6. Prosperity spell
7. Protection spell
8. Get a good job spell
9. Becoming a manager spell
10.Getting your scam money back
11. Are you suffering from a long time sickness
12. Freedom spell
13. Love spell
14. Court case spells
contact him now drhopespiritualhome@gmail.com or WhatsApp him +2348118045454 .
Friday, March 13, 2026
,DIABETES,CANCER,HPV,LOW SPERM COUNT, HIV/AIDS, FIBROSIS, LOSS OF WEIGHT .. all thank to you Doctor Razor for your kindly help in my life
Whatsapp him on +2349065420442. You are Indeed GOD SENT!! Visit his website https://herbalistrazorherb.wixsite.com/drrazorherbalhome and place your order Saturday, March 14, 2026
Sunday, March 15, 2026
Sunday, March 15, 2026
Email: illuminatireserves@gmail.com Sunday, March 15, 2026
Monday, March 16, 2026
Monday, March 16, 2026
Email: lordmeduzatemple@hotmail.com
Whats App: +1 807 798 3042.
Website: lordmeduzatemple.com Monday, March 16, 2026
.
Tuesday, March 17, 2026
ancientspellcast.wordpress.com
WhatsApp +2347070518515 Wednesday, March 18, 2026
1. Getting your lover or husband back
2. HIV/aids cure spell
3. Pregnancy spell
4. Money spell
5. Long life spell
6. Prosperity spell
7. Protection spell
8. Get a good job spell
9. Becoming a manager spell
10.Getting your scam money back
11. Are you suffering from a long time sickness
12. Freedom spell
13. Love spell
14. Court case spells
contact him now drhopespiritualhome@gmail.com or WhatsApp him +2348118045454 .
Wednesday, March 18, 2026
Wednesday, March 18, 2026
Email: drpeterspellcaster21@gmail.com
WhatsApp: +2348162247974
Website: drpeterspellcaster.wixsite.com/my-site-1 Wednesday, March 18, 2026
Email: drpeterspellcaster21@gmail.com
WhatsApp: +2348162247974
Website: drpeterspellcaster.wixsite.com/my-site-1 Wednesday, March 18, 2026
Beware of fabricated reviews and testimonies endorsing tricksters, do not get scammed because you seek for a genuine spell caster that will help solve and guarantee you result within the next 24hours, Depending on how serious and prepared you are to get your desired help here. We are approved spell caster by the authority to help people with any kind of situation, This is also to alert the public that our spell casting has no form of any side effect and is harmless. Our spell casting services is as follows:
*Relationship Spell
*Return an ex-lover spell
*Money spell to make you rich
*Spell to make you win any case in court
*Recover of lost money back from scammers
*Active spells to make you will lotteries
*Spell to cure anyone of any form of disease
*Spell to protect you from any form of danger
*Love spell to make anyone love you beyond control
*Restoring of your broken marriage, No matter how long you both have been separated
*Healing spells here to make you fine and well if you are sick. no matter any form of sickness.
No matter any spiritual/spell casting services you want on earth, Am giving you a more than 100% assurance that with our durable and tested and trusted spell casting services we will get it solved for you. Be happy again by using our spell casting services. Contact us via email: guduspells@gmail.com . Thursday, March 19, 2026
email, ebosehealer@ gmail . com Thursday, March 19, 2026
His WhatsApp: +2347046030096
Email: drisaspellcaster@gmail.com
Website: https://drisaspellcaster.wixsite.com/dr-isa Friday, March 20, 2026
I have been infected with Genital herpes for 1 year now , i have done so many medical treatments from different hospitals still
not cured.On a very good day , I decided making research onliner on how to get rid of Genital herpes, I found a post of Sarah Wilson on how she was cured from herpes with HERBALIST Sakura herbal remedy.
The Herbalist email was there as well drsakuraspellalter@gmail.com +2348110114739. I contacted him for my Genital herpes infection.
He needed a little of my information and also sent me his medicine through FedEx courier service.
I received it after 3 working days of shipment, I drank herbal medicine the same way Dr. Sakura instructed.
but now my Genital herpes is gone totally without any side effects or harm, may God Almighty continue to bless him abundantly .
you can contact him on mail/ what's-app dr.sakuraspellalter@gmail.com +2348110114739 or follow him on facebook @herbalist sakura health clinic@herbalist_sakura visit his website https://drsakurahealthclinic.wixsite.com/website
https://sites.google.com/view/herbalistsakura / you can as well contact me for more information celinagomez784@gmail.com Saturday, March 21, 2026
Website ancientspellcast.wordpress.com WhatsApp: +2347070518515 Saturday, March 21, 2026
Sunday, March 22, 2026
Sunday, March 22, 2026
Within weeks of the spell, my husband began to question his decision and eventually returned home. We’re now rebuilding our relationship, stronger than ever. I’m forever grateful to Dr ABDUL for their divine intervention. If you’re facing a similar situation, don’t give up hope Dr ABDUL can make the impossible possible! You can contact Dr ABDUL on the following contact address
Whatsapp +2.3.4.8.1.0.8.7.2.8.2.5.6 Monday, March 23, 2026
Within weeks of the spell, my husband began to question his decision and eventually returned home. We’re now rebuilding our relationship, stronger than ever. I’m forever grateful to Dr ABDUL for their divine intervention. If you’re facing a similar situation, don’t give up hope Dr ABDUL can make the impossible possible! You can contact Dr ABDUL on the following contact address
Whatsapp +2.3.4.8.1.0.8.7.2.8.2.5.6 Monday, March 23, 2026
Within weeks of the spell, my husband began to question his decision and eventually returned home. We’re now rebuilding our relationship, stronger than ever. I’m forever grateful to Dr ABDUL for their divine intervention. If you’re facing a similar situation, don’t give up hope Dr ABDUL can make the impossible possible! You can contact Dr ABDUL on the following contact address
Whatsapp +2.3.4.8.1.0.8.7.2.8.2.5.6 Monday, March 23, 2026
Within weeks of the spell, my husband began to question his decision and eventually returned home. We’re now rebuilding our relationship, stronger than ever. I’m forever grateful to Dr ABDUL for their divine intervention. If you’re facing a similar situation, don’t give up hope Dr ABDUL can make the impossible possible! You can contact Dr ABDUL on the following contact address
Whatsapp +2.3.4.8.1.0.8.7.2.8.2.5.6 Monday, March 23, 2026
oyaguherbalhome@gmail.com https://www.facebook.com/share/17BnC15B4i/ Monday, March 23, 2026
You can contact him on is email
drprogress1@gmail.com
Or mobile or WhatsApp number
+2348022830500 Monday, March 23, 2026
Wednesday, March 25, 2026
Wednesday, March 25, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Wednesday, March 25, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Wednesday, March 25, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Wednesday, March 25, 2026
You can reach them via email at H A C K M A V E N S 5 [AT] G M A I L [DOT] COM or [+] [1] [2 0 9] [4 1 7] – [1 9 5 7].
Wednesday, March 25, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Wednesday, March 25, 2026
Hello everyone my names are ALEX JACKSON from the UK, I want to use this golden medium to appreciate Doctor Abdul a great spell caster for helping me retrieving back my relationship with my ex lover when he ended and turned back on me for quite a long time now (6 months ago). He performed a spell for me and within 48 hours after the spell had been cast I received a text from my ex saying that he is sorry for the pains and tears that he had caused me and that he will not do such a thing to me again in his life. I was surprised but later accepted him back again. Anyone that is in the same line of problem or different one that wants to contact a spell caster should happily contact Doctor Abdul now on this email doctorabdulspellcaster@gmail. com or message him through his Whatsapp +2348108728256 Wednesday, March 25, 2026
HE ALSO RENDERED THE FOLLOWING …1. BRING YOUR EX BACK..2. LOTTERY SPELL.3. PREGNANCY SPELL .4. WEAK ERECTION 5. POOR EJACULATION...… Thursday, March 26, 2026
You can contact him on is email
drprogress1@gmail.com
Or mobile or WhatsApp number
+2348022830500 Thursday, March 26, 2026
HIV/AIDS,
SHINGLES,
CANCER,
HUMAN PAPILLOMA VIRUS,
ASTHMA,
DIABETES
BARRENNESS/INFERTILITY P*NIS ENLARGEMENTSPELL COUNSELING.
You Can decide to reach Herbalist Razor on his Email address : drrazorherbalhome@gmail.com . Cell Phone/Whatsapp Number +2349065420442 Friday, March 27, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I'm thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I'm forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461
Saturday, March 28, 2026
Sunday, March 29, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, March 30, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, March 30, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, March 30, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, March 30, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, March 30, 2026
Wednesday, April 1, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Wednesday, April 1, 2026
Wednesday, April 1, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Wednesday, April 1, 2026
PHONE/WHATS APP : +2347035623817 Wednesday, April 1, 2026
medicalmediumherbal@gmail.com
PHONE/WHATS APP : +2347035623817 Wednesday, April 1, 2026
medicalmediumherbal@gmail.com
PHONE/WHATS APP : +2347035623817 Wednesday, April 1, 2026
Thursday, April 2, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Thursday, April 2, 2026
Thursday, April 2, 2026
1: HIV/AIDS
2: HSV
3: LUPUS
4: ALS
5: HEPATITIS B
6: DIABETES
7: HUMAN PAPILLOMAVIRUS (HPV)
8: CANCER
9: GET YOUR EX BACK
10: PENIS ENLARGEMENT
11: THYROID ETC.
12 BACK TO SENDER SPELL
visit https://originalherbs.nicepage.io/ Friday, April 3, 2026
Do you want to hire a hacker to solve your problems in various conditions? If you require the services of a genuine hacker and do not have any idea about how to hire a professional hacker online, you are at the right place. There are many cryptocurrency theft cases and schemes currently in circulation in the whole world so it’s important to be careful before investing with any platform. I lost almost all my savings in a fake investment website but I got rescued through the recovery hacker called GEO COORDINATES RECOVERY HACKER as they recovered my stolen funds completely without hassle or hidden fees. This expert retrieved my stolen funds remotely within a few hours as I got notification on my blockchain wallet my funds had been restored. This is the best help I ever got on the internet and I decided to give them a good review about their good job and how quick the are in helping and standing for individuals in tough situations. Kindly contact them if you are in trouble.
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Friday, April 3, 2026
Friday, April 3, 2026
Friday, April 3, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Friday, April 3, 2026
Friday, April 3, 2026
Friday, April 3, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Friday, April 3, 2026
Saturday, April 4, 2026
Saturday, April 4, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Saturday, April 4, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Saturday, April 4, 2026
Saturday, April 4, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Sunday, April 5, 2026
There is an expert hacker that can help you in recovering all the money lost to scammers online. GEO COORDINATES RECOVERY HACKER It recently worked for me and I now have peace of mind after the huge recovery of all my lost funds. I’m truly grateful for their service and I recommend their service to everyone who needs to recover their stolen crypto funds. I will advise you to contact them with the details below.
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Sunday, April 5, 2026
There is an expert hacker that can help you in recovering all the money lost to scammers online. GEO COORDINATES RECOVERY HACKER It recently worked for me and I now have peace of mind after the huge recovery of all my lost funds. I’m truly grateful for their service and I recommend their service to everyone who needs to recover their stolen crypto funds. I will advise you to contact them with the details below.
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Sunday, April 5, 2026
There is an expert hacker that can help you in recovering all the money lost to scammers online. GEO COORDINATES RECOVERY HACKER It recently worked for me and I now have peace of mind after the huge recovery of all my lost funds. I’m truly grateful for their service and I recommend their service to everyone who needs to recover their stolen crypto funds. I will advise you to contact them with the details below.
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Sunday, April 5, 2026
There is an expert hacker that can help you in recovering all the money lost to scammers online. GEO COORDINATES RECOVERY HACKER It recently worked for me and I now have peace of mind after the huge recovery of all my lost funds. I’m truly grateful for their service and I recommend their service to everyone who needs to recover their stolen crypto funds. I will advise you to contact them with the details below.
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Sunday, April 5, 2026
Sunday, April 5, 2026
Sunday, April 5, 2026
Sunday, April 5, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Sunday, April 5, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Sunday, April 5, 2026
Sunday, April 5, 2026
medicalmediumherbal@gmail.com
PHONE/WHATS APP : +2347035623817 Monday, April 6, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Monday, April 6, 2026
finally breathing again. They didn’t just return money—they gave me back hope and also trust.
You can reach out to them at
Email : ghostchampionwizard@gmail.com
Telegram: https://t.me/WizardGhosthacker
Website : https://stellamariaqueen03.wixsite.com/-ghost-champion-wiza Monday, April 6, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, April 6, 2026
I’m thrilled to share my incredible experience with Dr Jakuta, a powerful spell caster who helped me reunite with my wife. We were facing numerous issues, and our relationship deteriorated, leading to a heartbreaking breakup. However, with the guidance of Dr Jakuta, whom my friend introduced me to, I followed his advice and, amazingly, my wife returned to me within 24 hours! I’m forever grateful. For those seeking help, you can reach Dr Jakuta at doctorjakutaspellcaster24@gmail. com or WhatsApp him on +2349161779461 Monday, April 6, 2026
Email: illuminatisaving@gmail.com Tuesday, April 7, 2026
Tuesday, April 7, 2026
Tuesday, April 7, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Tuesday, April 7, 2026
Wednesday, April 8, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Wednesday, April 8, 2026
Website: https://drlacocospellhome.wixsite.com/dr-lacoco Friday, April 10, 2026
I’m a US resident who contracted genital herpes from my ex-boyfriend, who showed no symptoms. Living with the condition for four years significantly impacted my life until I found a cure. I want to raise awareness that herpes is more than just a minor skin irritation; it has long-term health effects. Unfortunately, the stigma surrounding this virus is perpetuated by misinformation. In reality, many people have herpes in some form, often unknowingly. Personally, I found relief through Dr. Oosa medicine. Inspired by a testimonial from an Irish woman who cured her herpes with his help, I contacted Dr. Oosa. He assured me of a cure and provided his herbal medicine via DHL. Following his instructions, I took the medicine twice daily for six days. After completing the treatment, I was herpes-free, confirmed by my doctor. If you’re struggling with herpes or similar conditions and seeking a cure, consider contacting Dr. Oosa for guidance. Kindly contact doctor oosa via email: doctoroosaherbalhome@gmail.com whatsapp +2349066208065 Saturday, April 11, 2026
I’m a US resident who contracted genital herpes from my ex-boyfriend, who showed no symptoms. Living with the condition for four years significantly impacted my life until I found a cure. I want to raise awareness that herpes is more than just a minor skin irritation; it has long-term health effects. Unfortunately, the stigma surrounding this virus is perpetuated by misinformation. In reality, many people have herpes in some form, often unknowingly. Personally, I found relief through Dr. Oosa medicine. Inspired by a testimonial from an Irish woman who cured her herpes with his help, I contacted Dr. Oosa. He assured me of a cure and provided his herbal medicine via DHL. Following his instructions, I took the medicine twice daily for six days. After completing the treatment, I was herpes-free, confirmed by my doctor. If you’re struggling with herpes or similar conditions and seeking a cure, consider contacting Dr. Oosa for guidance. Kindly contact doctor oosa via email: doctoroosaherbalhome@gmail.com whatsapp +2349066208065 Saturday, April 11, 2026
I’m a US resident who contracted genital herpes from my ex-boyfriend, who showed no symptoms. Living with the condition for four years significantly impacted my life until I found a cure. I want to raise awareness that herpes is more than just a minor skin irritation; it has long-term health effects. Unfortunately, the stigma surrounding this virus is perpetuated by misinformation. In reality, many people have herpes in some form, often unknowingly. Personally, I found relief through Dr. Oosa medicine. Inspired by a testimonial from an Irish woman who cured her herpes with his help, I contacted Dr. Oosa. He assured me of a cure and provided his herbal medicine via DHL. Following his instructions, I took the medicine twice daily for six days. After completing the treatment, I was herpes-free, confirmed by my doctor. If you’re struggling with herpes or similar conditions and seeking a cure, consider contacting Dr. Oosa for guidance. Kindly contact doctor oosa via email: doctoroosaherbalhome@gmail.com whatsapp +2349066208065 Saturday, April 11, 2026
I would love to extend my gratitude and utmost appreciation to Geo Coordinates Hacker for helping me recover my money back. They helped me recover my stolen money, 634,000 dollars worth of bitcoin effortlessly. Their service is not only quick but professional and reliable. As someone who was skeptical about the process, I was pleasantly surprised to see my bitcoins returned in such a swift and hassle-free manner. Geo Coordinates Hacker truly goes above and beyond to ensure their clients' satisfaction. I would highly recommend Geo Coordinates Hacker for all your cryptocurrency recovery, digital funds recovery, hacking, and cybersecurity-related issues. Without a doubt, they are the best and I am very grateful to them for helping me recover my money. In case you have the same issues related to mine do not hesitate to reach out to them through their email Contact;
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Saturday, April 11, 2026
I would love to extend my gratitude and utmost appreciation to Geo Coordinates Hacker for helping me recover my money back. They helped me recover my stolen money, 634,000 dollars worth of bitcoin effortlessly. Their service is not only quick but professional and reliable. As someone who was skeptical about the process, I was pleasantly surprised to see my bitcoins returned in such a swift and hassle-free manner. Geo Coordinates Hacker truly goes above and beyond to ensure their clients' satisfaction. I would highly recommend Geo Coordinates Hacker for all your cryptocurrency recovery, digital funds recovery, hacking, and cybersecurity-related issues. Without a doubt, they are the best and I am very grateful to them for helping me recover my money. In case you have the same issues related to mine do not hesitate to reach out to them through their email Contact;
Email: geovcoordinateshacker@gmail.com
Website; https://geovcoordinateshac.wixsite.com/geo-coordinates-hack
Saturday, April 11, 2026
I’m truly grateful to them, as my crypto was recovered shortly after I got in touch, their team was very supportive. Morphohack helped me bounce back from what was a terrible loss. You can contact them via email at(Morphohack@cyberservices.com) Monday, April 13, 2026
I was at work the next morning when my friend FaceTimed me and asked me if I had checked my ticket because the news was saying the winning ticket was bought at the Huron Plaza Liquor.
I got off the phone and went to my truck to get the ticket. After I checked it, all could do was scream. Everyone from work came running to check on me. Once I got calmed down, my boss made sure I was able to get a ride home because there was no way I would be able to drive after learning I was a multi-millionaire. thank you so much Dr Dominion for what you have done for my entire generations, i will forever be grateful. you may want to try him too here is his info bellow:
Email: dominionlottospelltemple@gmail.com
website: dominionlottospell.wixsite.com/dr-dominion
phone: +12059642462 Thursday, April 16, 2026
Thank you! Dr. Excellent brought my husband back to me today.
I can’t think of anything more painful or heartbreaking than hearing your husband say “I don’t love you anymore. Or “It’s over. I’m in love with someone else.”
My name is Heather Delaney. I married the love of my life Riley on 10/02/15 and we now have two beautiful girls Abby & Erin, who are conjoined twins, that were born 07/24/16. My husband left me and moved to be with another woman. I felt my life was over and my kids thought they would never see their father again. I tried to be strong just for the kids but I could not control the pains that tormented my heart, my heart was filled with sorrows and pains because I was really in love with my husband. I have tried many options but he did not come back, until i met a friend that directed me to Dr. Excellent a spell caster, who helped me to bring back my husband after 11hours. Me and my husband are living happily together again, This man is powerful, contact Dr. Excellent if you are passing through any difficulty in life or having troubles in your marriage or relationship, he is capable of making things right for you. Here his contact. Call/WhatsApp him at: +2348084273514 "Or email him at: Excellentspellcaster@gmail.com ,For more information visit his website:https://drexcellentspellcaster.godaddysites.com
Friday, April 17, 2026
Thank you! Dr. Excellent brought my husband back to me today.
I can’t think of anything more painful or heartbreaking than hearing your husband say “I don’t love you anymore. Or “It’s over. I’m in love with someone else.”
My name is Heather Delaney. I married the love of my life Riley on 10/02/15 and we now have two beautiful girls Abby & Erin, who are conjoined twins, that were born 07/24/16. My husband left me and moved to be with another woman. I felt my life was over and my kids thought they would never see their father again. I tried to be strong just for the kids but I could not control the pains that tormented my heart, my heart was filled with sorrows and pains because I was really in love with my husband. I have tried many options but he did not come back, until i met a friend that directed me to Dr. Excellent a spell caster, who helped me to bring back my husband after 11hours. Me and my husband are living happily together again, This man is powerful, contact Dr. Excellent if you are passing through any difficulty in life or having troubles in your marriage or relationship, he is capable of making things right for you. Here his contact. Call/WhatsApp him at: +2348084273514 "Or email him at: Excellentspellcaster@gmail.com ,For more information visit his website:https://drexcellentspellcaster.godaddysites.com
Friday, April 17, 2026
Sunday, April 19, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Sunday, April 19, 2026
Friday, April 24, 2026
Facebook page : https://facebook.com/drsikies
Make order now via website https://drsikiesherbalcuremedicine.weebly.com/
Friday, April 24, 2026
Saturday, April 25, 2026
https://www.facebook.com/dr.agbominanaturalcure Saturday, April 25, 2026
Sunday, April 26, 2026
https://www.facebook.com/dr.agbominanaturalcure Monday, April 27, 2026
I've gotten sores since I was a kid. At it's worst, I had 25 in one year. Typically I get around 8-12 a year. That is with years of prescription medication, lysine, topicals, etc. My cold sores have typically been on the smaller side since I take medication, but very frequent. one day I was searching the internet and I came across a testimony of someone saying DR GOOD HEALTH REMEDY Cured her from Genital herpes, I was a bit skeptical about it but I decide to give it a try and today my herpes virus is also cured totally. thank you DR GOOD HEALTH For your cure I am grateful. you can Contact him with the following details. Email: drpowerherbalremedycure@gmail.com or WhatsApp him on +2349069180178
WEBSITE:https://drpowerherbalremedycure.wordpress.com/ Tuesday, April 28, 2026
I've gotten sores since I was a kid. At it's worst, I had 25 in one year. Typically I get around 8-12 a year. That is with years of prescription medication, lysine, topicals, etc. My cold sores have typically been on the smaller side since I take medication, but very frequent. one day I was searching the internet and I came across a testimony of someone saying DR GOOD HEALTH REMEDY Cured her from Genital herpes, I was a bit skeptical about it but I decide to give it a try and today my herpes virus is also cured totally. thank you DR GOOD HEALTH For your cure I am grateful. you can Contact him with the following details. Email: drpowerherbalremedycure@gmail.com or WhatsApp him on +2349069180178
WEBSITE:https://drpowerherbalremedycure.wordpress.com/ Tuesday, April 28, 2026
Friday, May 1, 2026
https://www.facebook.com/Spiritual_spell_temple_1111-100570192704287 Friday, May 1, 2026
(+2348056484618) email himon: Luckyseph1113@gmail.com, For immediately response… My Regard to Mr Joseph Lucky .............. Friday, May 1, 2026
Saturday, May 2, 2026
You can also reach doctor UMA on WhatsApp
+2347035619585 or Email dr.umaherbalcenter@gmail.com.
Saturday, May 2, 2026
Thursday, May 7, 2026